Glaucoma is a term that is used to describe a broad range of eye problems that can damage the optic nerve and cause loss of vision. The pressure inside the eye, called Intraocular Pressure (IOP), generally falls within a range that is considered “normal.” Many patients believe that Glaucoma is simply due to a high pressure within the eye.
While high Intraocular pressure is the most common cause of Glaucoma, a high IOP may not be the only cause of Glaucoma. Regardless of the cause, the various types of Glaucoma share a common factor: if not diagnosed early, treated properly, and controlled, it will result in permanent vision loss and potentially blindness. Dr. Spector is a Fellowship trained Glaucoma specialist and provides comprehensive diagnostic testing and treatment for Glaucoma.
Types Of Glaucoma
Primary Open Angle Glaucoma
The most common type of Glaucoma is Primary Open Angle Glaucoma (POAG). In the “normal” eye, there is a continuous production and drainage of a clear colorless fluid called “Aqueous Humor.” This production and drainage is balanced so that an equal amount is produced and drained to maintain an equilibrium, resulting in a “normal’ Intraocular Pressure (IOP). Patients with Primary Open Angle Glaucoma usually have an increase in Intraocular Pressure (IOP) upon routine measurement.
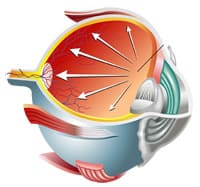
In the event that there is either too much Aqueous Humor being produced or too little Aqueous Humor is being drained, there is a rise in pressure inside the eye. Any elevation of Intraocular Pressure (IOP) is considered “abnormal.” This elevation in pressure (IOP) causes the circulation in the optic nerve to become compromised, depriving it of oxygen and nutrients, resulting in permanent changes and even damage to the optic nerve. The optic nerve is the connection responsible for communicating visual images between the retina and the brain. When the optic nerve is damaged, it is not able to carry visual images, resulting in vision loss. This is why it is so important to monitor, detect and control Intraocular Pressure (IOP). If left untreated, an elevated Intraocular Pressure (IOP) may, over time, cause slow, progressive and permanent damage to the optic nerve that can result in blindness.
Angle Closure Glaucoma
Angle Closure Glaucoma is characterized by a blockage or complete closure of the drainage structure of the eye called the Trabecular Meshwork. The Trabecular Meshwork is a fine filter. If it is blocked or obstructed by any alteration in the size or shape of the surrounding structures, or by change in the size or shape of the tissue itself, it will cause the Intraocular Pressure to elevate. Angle Closure Glaucoma can be divided in two main types: Primary Angle Closure Glaucoma and Acute Angle Closure Glaucoma. Primary Angle Closure Glaucoma accounts for approximately 10% of all cases of Glaucoma and about 2/3 of these produce no symptoms for patients. Although Angle Closure Glaucoma occurs much less frequently than Open Angle Glaucoma, it is important to understand it because it has the ability to produce considerable vision loss in a short period of time.
In instances where the Meshwork becomes blocked abruptly, it will cause a sudden rise in the Intraocular Pressure (IOP), resulting in Acute Angle Closure Glaucoma. Acute Angle Closure Glaucoma is characterized by this sudden rise in pressure which can cause pain, redness, light sensitivity, colored halos around lights, nausea or vomiting and blurred vision, and, if left untreated, permanent loss of vision. While there can be several causes of Angle Closure Glaucoma, it is most often caused by anatomical changes within the internal structures of the eye. Angle Closure Glaucoma is considerably more common in farsighted eyes, which tend to be smaller and in patients between the ages of 45-60 years of age where the Crystalline Lens is beginning to swell.
Acute Angle Closure Glaucoma is considered a medical emergency. If you experience a sudden onset of pain, redness, blurred vision, light sensitivity, halos around lights, nausea and vomiting, please call Spector Eye Care at 203-853-9900 and relay these symptoms to the receptionist so that you can be given an appointment immediately.
Other Types
Sometimes it is possible to have damage to the optic nerve, even with a “normal” Intraocular Pressure (IOP). When optic nerve damage has occurred despite a normal IOP, this is called Normal Tension Glaucoma.
Secondary Glaucoma refers to any case in which another disease causes or contributes to increased eye pressure, resulting in optic nerve damage and vision loss.
During your routine eye exam if one of the eye doctors observes or measures a narrowed angle, he or she will perform an additional examination procedure called Gonioscopy. This will allow the doctor to directly examine the Trabecular Meshwork and the angle in order to carefully assess your predisposition to Angle Closure Glaucoma. By placing a special contact lens on your eye and using the slit lamp biomicroscope to fully examine the meshwork and the angle, with Gonioscopy the doctor will be able to make a thorough evaluation.

Causes
Everyone is at risk for Glaucoma. However, depending on your general health, eye health and other family history considerations, there are several factors that may influence your likelihood of developing Glaucoma. These “Glaucoma Risk Factors” are important to understand in assessing your own personal risk for developing Glaucoma. Glaucoma risk factors include the following:
- High Intraocular Pressure
A key warning sign of Glaucoma is having a higher than normal Intraocular Pressure (IOP). Anyone with an elevated Intraocular Pressure (IOP) is considered at risk for developing Glaucoma.
- Age
There is a direct relationship between age and the likelihood of developing Glaucoma. The chances of developing Glaucoma increase considerably after the age of 40, and you are six times more likely to get Glaucoma if you are over 60 years of age, even if you have no other relevant family or medical history.
- Race
Race plays a significant role in the likelihood of developing Glaucoma. Glaucoma is the leading cause of blindness in the Black Community because certain genetic factors cause a six to eight-fold increase in risk for Glaucoma. People of Asian descent appear to have higher risk for developing Narrow Angle Glaucoma. In addition, people over the age of 60 in the Hispanic and Latino Communities seem to be at increased risk as well.
- Myopia
Certain patients who are severely nearsighted have a higher risk of developing Glaucoma due to certain anatomical features in eyes with Myopia.
- Hypertension or High Blood Pressure
It is critical that patients who have hypertension or high blood pressure take their prescribed medication on a consistent basis. However, patients who take medication for high blood pressure may be at greater risk for Glaucoma as a result of the medication lowering the blood pressure and thus decreasing circulation within the optic nerve.
- Diabetes
Diabetes can cause general problems with circulation throughout the body, including the eye. As a result of the poor circulation, patients with diabetes are considered at greater risk for developing Glaucoma.
- Family History
Any family history of Glaucoma is considered a very significant risk factor. If any members of your family have been diagnosed with Glaucoma, it increases the likelihood that you will develop Glaucoma by 4-9 times over the general population. This is particularly true for siblings of Glaucoma patients who have a 5-fold increase in risk for developing Glaucoma.
In addition to these factors, if you have had trauma to your eyes (i.e. a sports injury or car accident), or if you have been treated for Asthma for long periods of time with steroid inhalers, or if you have a corneal thickness less than .5mm, you may have an increased risk for Glaucoma.
Symptoms
There are typically no early warning signs or symptoms of open-angle glaucoma. It develops slowly and sometimes without noticeable sight loss for many years. Most people who have open-angle glaucoma feel fine and do not notice a change in their vision at first because the initial loss of vision is of side or peripheral vision, and the visual acuity or sharpness of vision is maintained until late in the disease. By the time a patient is aware of vision loss, the disease is usually quite advanced. Vision loss from glaucoma is not reversible with treatment, even with surgery.
Symptoms of acute angle-closure glaucoma are very noticeable, and damage occurs quickly. Symptoms include hazy or blurred vision, the appearance of rainbow-colored circles around bright lights, eye and head pain, nausea or vomiting (accompanying severe eye pain), sudden sight loss. In angle-closure glaucoma, the angle is closed in many or most areas, causing increased eye pressure, which leads to optic nerve damage, and possible vision loss.
Treatment
Glaucoma has no cure, but in almost all cases, it is treatable if caught early. As a Glaucoma Specialist, there are three main methods that Dr. Spector can use to treat Glaucoma: Medical, Laser and Surgical.
Primary Open Angle Glaucoma is most often treated with eye drops. There are many types of eye drops that can be prescribed to lower Intraocular Pressure (IOP). By using a single type of medication or sometimes 2 eye drops in combination, more than 80% of the patients with Open Angle Glaucoma can be successfully treated.
Dr. Spector has found that the use of Laser Treatment for Glaucoma has become an important option for many patients. In the past, Laser Eye Surgery for Glaucoma was considered a “last resort” before Glaucoma Surgery. Today, thanks to advances in lasers, using a laser treatment for Glaucoma in conjunction with the eye drop treatment or sometimes even using the Laser Treatment as the primary treatment are excellent options to help maintain control and slow or stop the progression of the disease.
For a small number of patients, it is still not possible to achieve control of their disease and stop the progression of vision loss, even with the maximum medical therapy they can achieve with Glaucoma eye drops and Laser Eye Surgery. For these patients, Dr. Spector can perform several surgical procedures, including: Trabeculectomy, wherein a tiny piece of the Trabecular Meshwork is removed, Sclerostomy or “Filtering Procedure”, which removes a small piece of the sclera for drainage, or even implanting a microscopic Glaucoma Valve to help reduce and stabilize the Intraocular Pressure (IOP).
For more information on the treatment options for Glaucoma, follow this link.