About The Cornea
The Cornea is an important structure of the eye that functions in a number of ways to help provide clear vision. First, it acts as the clear outermost “lens” of the eye that allows light rays to pass through to the Retina. Normally it is about the size and thickness of a dime and is curved in a dome like shape. It is critical for the Cornea to maintain its transparency and optical clarity as well as its regular curvature and thickness in order to function properly. When light strikes the cornea, it bends–or refracts–the incoming light onto the Crystalline Lens of the eye. The Crystalline Lens further focuses that light onto the Retina, a layer of light sensing cells lining the back of the eye.

For you to see clearly, light rays must be focused by the Cornea and Crystalline Lens to fall precisely on the Retina. The Retina takes that light energy, and makes it something the brain interprets as vision.
The Cornea also serves as a filter, screening out some of the most damaging ultraviolet (UV) wavelengths in sunlight. Without this protection, the Lens and the Retina would be highly susceptible to injury from UV radiation. Last, the Cornea serves to protect the internal structures of the eye by shielding it from easy penetration of microorganisms, dust and debris.
There are a number of eye diseases, conditions or problems that can affect the functioning of the cornea and thus your ability to see clearly. These can include: eye injuries, eye infections, inherited familial or genetic conditions, and aging changes. It is often possible to treat these conditions with eye drops or other medications, various types of surgery or contact lenses. In the event the cornea is badly compromised and non-surgical options do not help to improve vision, it may be necessary to have a Corneal Transplant.
About Corneal Infections
The outermost layer of the Cornea is called the epithelium. If it is damaged from trauma of any type, i.e. getting a foreign body in your eye such as piece of metal, a poke in the eye from a branch or a finger or even from a dirty or damaged contact lens, it is possible for bacteria, viruses or fungi to penetrate the Cornea and cause an infection. An infection of the cornea is called a Keratitis or Ulcer. Keratitis can cause a painful inflammation with a discharge, which if not treated quickly and appropriately, can lead to corneal erosion, corneal ulceration and corneal scarring. Corneal scarring results in a loss of corneal transparency and can require a corneal transplant in order to restore vision. Generally, the deeper the corneal infection, the more severe the symptoms and the greater the potential for loss of vision.
If your doctor suspects that you have a corneal infection, we will look for certain diagnostic signs to help decide the best course of treatment for corneal infections. Sometimes this might be an antibiotic eye drop, an antifungal eye drop, an antiviral eye drop and sometimes it might even include a steroid eye drop to reduce the inflammation.
About Herpes Zoster Keratitis (Shingles)
Herpes Zoster Keratitis is actually caused by the same virus that causes chicken pox, called Varicella-Zoster Virus. It is entirely possible that after having chicken pox as a child, the Varicella-Zoster Virus remains in the nerve cells of your body in an inactive state. For a number of possible reasons, the Varicella-Zoster Virus can reactivate later in life and travel through the nerves in your body causing a painful blistering rash. If the Varicella-Zoster Virus travels to your head or neck it can affect the eye and thus cause a corneal infection.
It is critical to have a Spector Eye Care doctor diagnose this quickly as the infection can penetrate deeply into the cornea and it can cause scarring. The infection can also result in a loss of corneal sensation, which can be permanent. Your doctor may prescribe both oral medications and eye drops to try and resolve the infection and prevent serious damage from occurring.
It is possible for anyone who has been exposed to the Varicella-Zoster Virus to get shingles, however it seems to affect those of advanced age and those with weakened or suppressed immune systems many times more often. Further, corneal problems from shingles may occur many months after the facial shingles appear to have resolved. Therefore, if you have had facial shingles it is important for you to schedule regular follow up appointments with Spector Eye Care.
About Ocular Herpes
Ocular Herpes, or Herpes of the eye is caused by the Herpes Simplex Virus and is the most common causes of corneal blindness in the United States today. Up to 50% of people who have a single Herpes Simplex viral infection of the eye will experience a flare up or recurrence. The virus often leads to irreversible scarring of the cornea.
Ocular Herpes may start as a painful sore on the eyelid or surface of the eye. If left untreated, it may multiply and begin to destroy epithelial cells and progress deeper into the cornea. If the Ocular Herpes penetrates the deeper layers of the cornea and causes a Stromal Keratitis it may cause corneal scarring-so prompt diagnosis and treatment of Ocular Herpes is important.
It is estimated that 400,000 people in the United States have had some type of Ocular Herpes, with more than 50,000 initial and recurring cases being diagnosed each year. Of these, it is believed that 25% are the more severe form of Herpes Stromal Keratitis. The recurrence of Herpes Simplex eye infections is significant in that it appears to recur in about 10% of patients with one year, 23% of patients within two years and 63% of patients within 20 years of their initial infection. Sometimes a recurrence can be prompted by sunlight, stress, fevers or an unrelated eye injury.
Our physicians may prescribe both oral medications and eye drops to try and resolve the infection and prevent serious damage from occurring. Prompt diagnosis and medication is key to preventing any vision loss.
About Corneal Dystrophies
Fuch’s Dystrophy is a slowly progressive disease of the cornea that can be found in both eyes and is slightly more common in women than men. While it is possible to observe Fuch’s Dystrophy in people in their 30’s and 40’s, it usually does not compromise vision until people are in their 50’s or 60’s. The innermost layer of cells in the cornea, called the endothelium, is a single layer of non-regenerating cells. The endothelial cells are responsible for pumping water out of the cornea and helping to maintain the corneal transparency. While the reason is poorly understood, in Fuch’s Dystrophy, the endothelial cells die, which make the endothelium less efficient in its pumping activity. This results in the cornea swelling and distorting vision. In its later phases, Fuch’s Dystrophy is often associated with considerable pain as the epithelium “blisters” by forming “bullae”, which actually begin to burst open.
Early in the course of Fuch’s Dystrophy patients will wake up with blurry vision that gets progressively clearer as the day passes. This phenomenon occurs because the cornea normally takes on water and swells during sleep. A healthy endothelial pump is necessary in order to restore the cornea to a normal thickness. In Fuch’s Dystrophy, the endothelium removes fluid from the cornea less efficiently. As the Fuch’s Dystrophy disease worsens and the vision does not clear, your doctor will attempt to help reduce the corneal swelling each day with eye drops and ointments. However, when these measures fail to provide comfort and clear vision, it may be necessary to have a Corneal Transplant.
About Map-Dot-Fingerprint Dystrophy
The outermost layer of the cornea, called the epithelium, is attached or anchored to an underlying basement membrane, called Bowman’s Membrane, in order to remain healthy. Sometimes the epithelial basement membrane develops abnormally making it difficult or impossible for the epithelium to adhere properly to the basement membrane. If the epithelium does not adhere properly, Recurrent Corneal Erosions will occur. Recurrent Corneal Erosions are painful and cause the corneal surface to become irregular resulting in intermittent blurry vision along with the discomfort and foreign body sensation. Map-Dot-Fingerprint Dystrophy is also known as Epithelial Basement Membrane Dystrophy because it is caused by a lack of the healthy formation of the Basement Membrane. It affects adults between the ages of 40-70 and can sometimes begin earlier. As the name implies, its appearance is of a map of gray areas, which may also be accompanied by opaque dots, and fingerprint like whirls or lines.
Your Spector Eye Care doctorwill often discover Map-Dot-Fingerprint Dystrophy during a routine eye examination in patients who do not have any noticeable symptoms. If treatment is required to control the pain for those patients who are symptomatic, Your doctor may prescribe lubricating eye drops, patch the eye, apply a soft bandage contact lens or in more severe cases, scrape the cornea to attempt to achieve better adhesion of the epithelium. In some cases, your doctor may suggest that the best results can be achieved using Excimer Laser Phototherapeutic Keratectomy (PTK) to smooth the surface of the cornea.
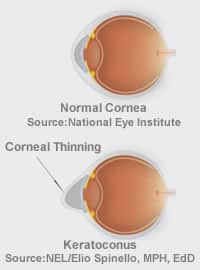
About Keratoconus
Keratoconus is disorder of the cornea characterized by a progressive thinning of the tissue, and instability of the cornea. The cornea begins to bulge outward and become cone-like. It is the most common corneal dystrophy found in the in the United States. As the cornea begins to bulge it causes considerable changes in the refractive power of the eye producing nearsightedness and astigmatism. Keratoconus usually affects both eyes. At first it may be possible to correct your vision with contact lenses. Unfortunately, for about 20% of patients, contact lens intolerance develops making a corneal transplant necessary.
For some patients, Intacs® Corneal Implants may be recommended for Keratoconus as an intermediate treatment between contact lenses and a Corneal Transplant. Intacs® prescription inserts are an option between contacts and a Corneal Transplant that may help to stabilize the cornea and improve vision. Intacs® prescription inserts are indicated for use in the correction of nearsightedness and astigmatism for patients with Keratoconus, where contact lenses and glasses are no longer suitable.
Your doctor will take all the time necessary to explain the various treatment options available. Please be assured that all of your questions will be answered so that you can make an educated and informed decision about your treatment options at Spector Eye Care.
About Other Corneal Conditions
Atachment of the outermost layer of the cornea, the epithelium, to the underlying basement membrane layer, called Bowman’s Membrane. Patients who experience Recurrent Corneal Erosion may experience sharp pain, light sensitivity, tearing and watering of their eyes, and a gritty sensation. Often this occurs upon awakening or rubbing the eyes. Recurrent Corneal Erosion is a condition that may be associated with Map-Dot-Fingerprint Dystrophy. Your doctor may initially prescribe salt solution eye drops or ointment as the first line of treatment. This medication helps the epithelium to adhere more firmly to Bowman’s Membrane. Usually artificial tears are also recommended to keep the cornea moist. Sometimes, a soft bandage contact lens will be used to help the healing process.
Those patients who have a corneal dystrophy may require additional treatment. This usually includes an in-office procedure where the epithelium is either gently removed, or microscopic “spot welds” are made on the cornea to encourage the epithelial layer to bond securely to Bowman’s Membrane.
Patients, who continue to suffer from Recurrent Corneal Erosions despite the treatments described, may benefit from Phototherapeutic Keratectomy (PTK). This involves removal of the superficial layer of corneal cells using the Excimer Laser to encourage proper healing.
Early Diagnosis And Treatment Is Essential
As you can see there are many conditions that can affect the cornea. Our team can often treat most of these eye conditions and corneal diseases using non-surgical treatment options. However if they are not diagnosed and treated early or if they progress to where vision is compromised beyond an acceptable level, it may be necessary for an ophthalmologist to perform a Corneal Transplant.